In a 6-month pilot, West Virginia University’s Ruby Memorial Hospital saw Top Box response rates increase by 3.5% for Pilot units while the rest of the hospital saw this rate decline by 1.6%. Using predictive analytics, APEXamenity quickly identifies patients who are least likely to have their issues resolved before leaving the hospital, so that PPE staff can intervene and resolve issues for silent saboteurs.
INTRODUCTION
West Virginia University’s Ruby Memorial Hospital completed a 6-month pilot of the APEXamenity Rounding Tool between March 5, 2019 and August 2019. Three pilot units were assigned to use the APEXamenity tool while the rest of the hospital pursued 100% rounding. Performance during the pilot was compared to the 12 months preceding the pilot.
RESULTS
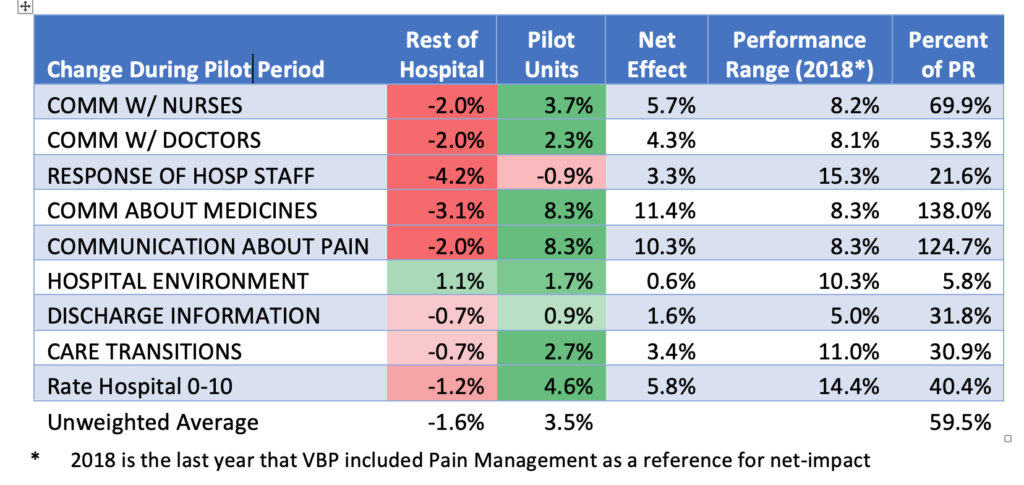
During the pilot period, pilot units showed a 3.5% increase on average for the 9 VBP-relevant HCAHPS Dimensions. The rest of the hospital saw a 1.6% decline on average over the same period. VPB Performance Ranges (i.e. the difference between Benchmark and Threshold) is an excellent way to put these changes in context, demonstrating the potential impact of APEXamenity on a hospital’s ranking, stars, and reimbursement.
LEVERAGING YOUR LEADERSHIP
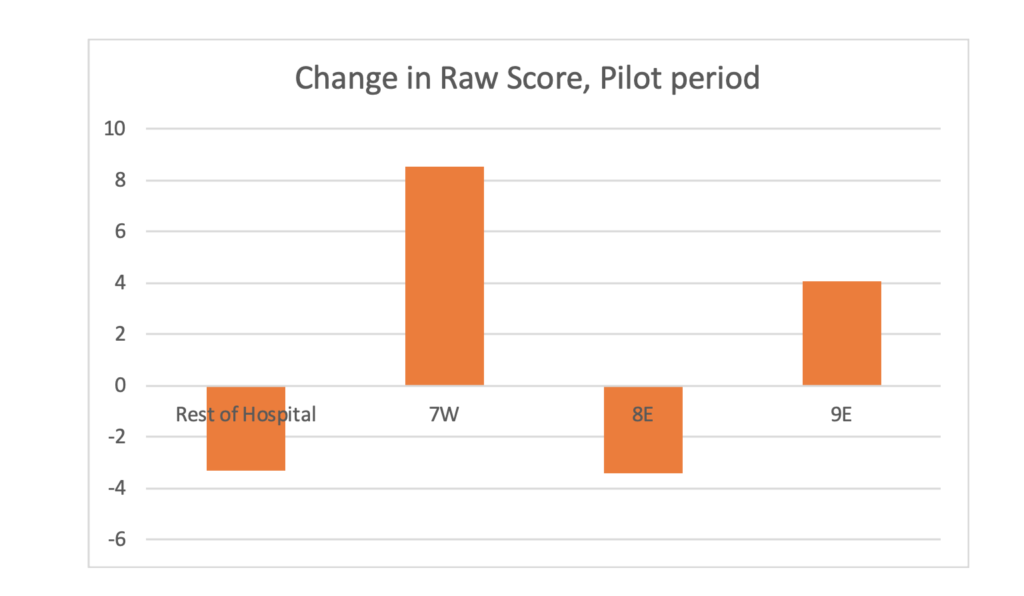
The story is even more striking when the impact of APEX on individual units is visualized.
Two units successfully engaged with APEX to produce significant, positive impacts for their units, in both absolute terms and relative to hospital-level declines. The third unit experienced a change in leadership – the leader who was to use the APEX tool – and produced results identical to the overall hospital. The data in the previous section actually includes this no-change unit and the unit’s performance actually supports the idea that the engagement between leadership and the tool was the driving force behind the success of the other pilot units.
Improving HCAHPS Through Predictive Analytics
APEXamenity achieves this impact by leveraging proprietary predictive models to identify patients who are least likely to have their issues resolved before leaving the hospital, producing not-top-box responses on the HCAHPS survey. On admission, patients in the pilot units are automatically run through these models and the results are forwarded to the APEXamenity tool for use by Nurse Leaders:
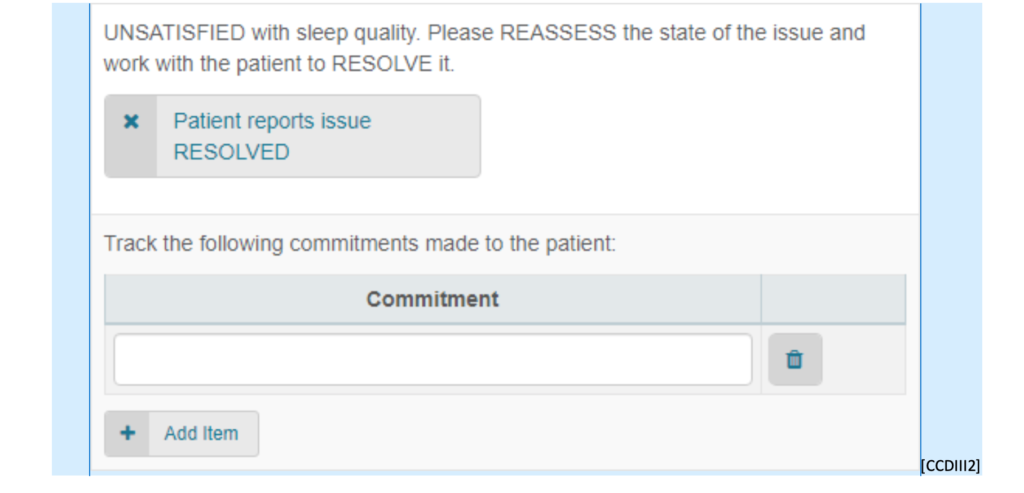
As Nurse Leaders engage patients, they track the patient’s responses and any commitments made to that patient:
GIVING THE SILENT SABOTEUR A VOICE
One of the most interesting aspects of the pilot was a perception by the Nurse Leaders that they weren’t talking to the right people – despite the significant and positive impact on scores. Every unit has a couple of patients who are vocal about their issues. In units with regulars, they may even know these patients by name. Why wouldn’t the model identify these “obvious” patients? The answer is both simple and heartening: Nurse Leaders are good at their job. When they identify a patient who is unsatisfied, they’re usually successful addressing that concern.
It follows that the majority of not-top-box respondents are actually patients who were not identified by a Nurse Leader. While less-than-100% rounding is certainly a possible explanation, we believe that many of these respondents are actually reticent to complain to Nurse Leaders. The patients may be averse to conflict, may not feel they are qualified to complain about the performance of a medical professional or may fear some sort of retaliation if they complain about the person wielding the needle. Whatever their reasons, these Silent Saboteurs often go undiscovered and unaddressed until they complete an “anonymous” HCAHPS survey.
APEXamenity helps to give these Silent Saboteurs a voice by prompting staff to be extra sensitive to the reaction of patients who are likely to fall into this category. If a high-risk patient says that everything is “OK” (vs. good or great), it may be a red flag that there is a latent issue. Nurse Leaders can help overcome this reticence by asking again or by trying to break the ice with a weaker statement like “We know we’re not perfect; what is one place we could improve?” Once the ice is broken, it’s easier to get to a patient’s actual concerns.
And this is exactly what Ruby experienced during their kick-off. As part of their training, three teams were sent to three different patients flagged as high risk. Two returned reasonably quickly with nothing to report, but one of the three was slow to return. When the team finally returned, they shared their experience. At first, the patient reported no issues. With a little persistence, however, the patient turned into a “gusher” (their words) reporting a wide variety of concerns and issues that they were then empowered to address.
Ambassador Software Works
Ambassador Software Works provides AI-based patient insights through its proprietary APEXamenity Rounding Tool and through partnerships with leading Rounding Tool vendors. To learn more about how AI-based patient insights can improve your patients’ experience, HCAHPS scores, and VBP reimbursement, please call 855.349.4224 or email sales@ambsw.com.